Share this article
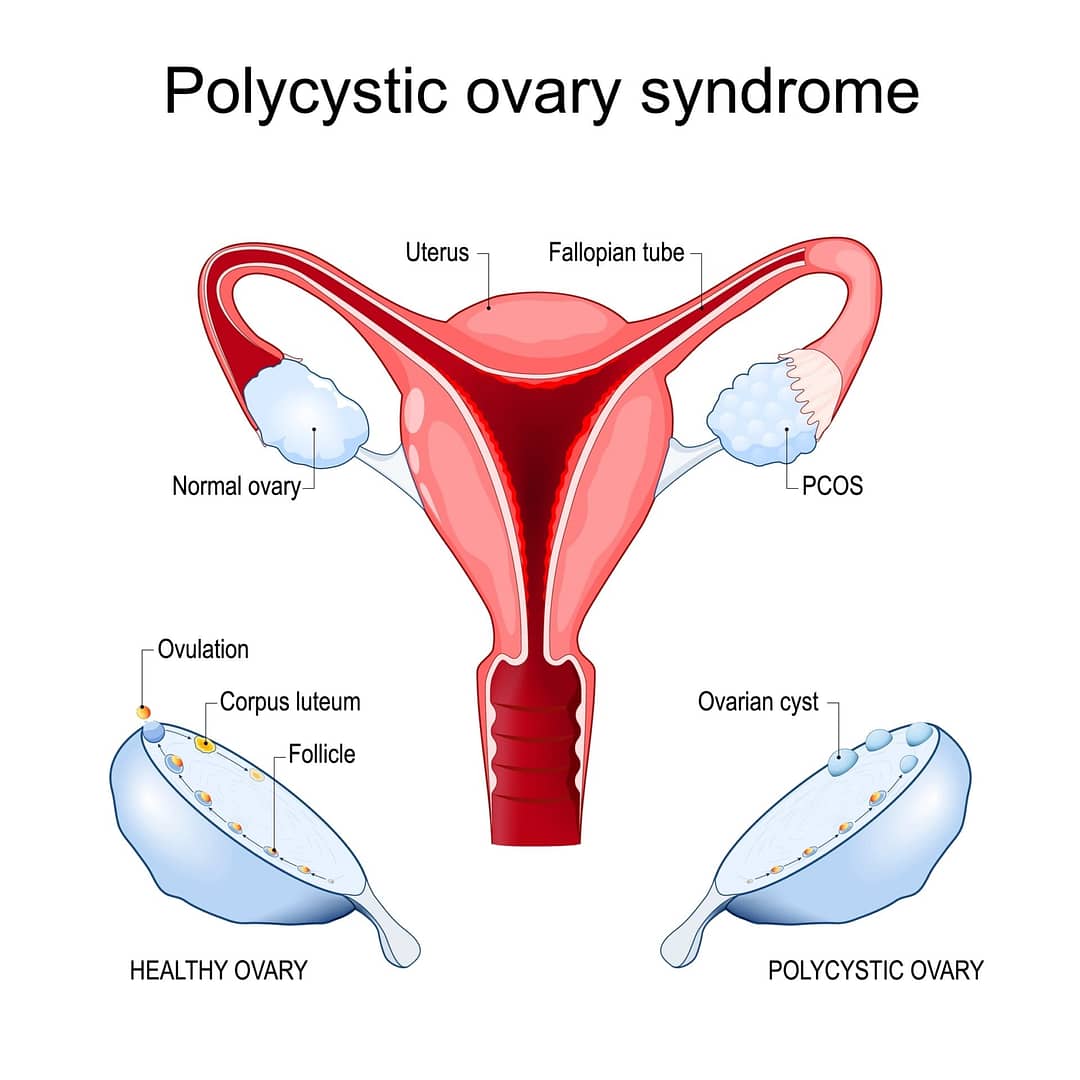
Polycystic Ovary Syndrome (PCOS) is a pervasive and intricate disorder of the endocrine system. PCOS happens when there is overproduction of androgens which interfere with the development of eggs and their release from the female ovaries. Therefore PCOS is a leading cause of infertility worldwide.
The disorder may be triggered by external factors such as stress or issues within the body such as insulin instability (Deswal et al, 2020, Healthdirect Australia, n.d.).
Since PCOS is accompanied by hyperandrogenism, hirsutism, abdominal obesity, increased body mass index (BMI) and waist to hip ratio (WHR), many woman face physical, and emotional challenges. To comprehend the true nature of this syndrome, it is crucial to delve into its origins and explore its effects on a woman’s body.
Understanding PCOS and The Symptoms That Come With It
PCOS is a multifaceted condition that arises from a combination of genetic and environmental factors. The primary culprits include insulin resistance(IR) due to a sedentary lifestyle and unhealthy eating habits, hormonal imbalances, and inflammation. In women with PCOS, the ovaries produce higher levels of androgens (male hormones) than usual, disrupting the normal menstrual cycle and leading to the formation of small cysts on the ovaries. This starting point opens up what essentially is a can of worms and leads the body’s homeostasis to go out of control.
Effects on a Woman’s Body
The effects of PCOS are far-reaching. Irregular menstrual cycles where periods are missed or come with agonisingly painful cramps, acne even in adults, excessive hair growth in the chin and neck area, and weight gain (especially gaining a significant amount of weight during a short period of time) are common short-term effects, while long-term consequences may include diabetes due to insulin complications, cardiovascular disease, and infertility. The excessive androgen production can lead to disrupted ovulation, hindering the release of mature eggs and causing fertility challenges. Some women resort to many treatments such as In-Vitro Fertilisation (IVF) to overcome the obstacle and hurdle of fertility due to PCOS.
Factors Contributing to PCOS
Several factors contribute to the development of PCOS, making it a complex interplay of genetics, lifestyle factors including stress, a sedentary lifestyle with little movement, an unbalanced diet with processed food, high sugar and environmental elements. Women with a family history of PCOS or those with sedentary lifestyles and poor dietary habits are more at risk to this condition and should take preventative measures. Early detection of PCOS will help women to manage symptoms or reverse the condition.
Demographics and Prevalence
PCOS does not discriminate and can affect women of all races and ethnicities, but some ethnic groups (Liu et al., 2021) may be more prone to it. PCOS often rears its ugly head during the reproductive years, with symptoms becoming apparent during adolescence or early adulthood.
Effects on Fertility, Periods, Hormones, and Weight
PCOS significantly influences fertility, as irregular ovulation can impede conception. Menstrual irregularities, such as missed or infrequent periods, are common and these women find it difficult to track their menstrual cycle. Hormonal imbalances contribute to acne, excessive facial and body hair growth (hirsutism), and male-pattern baldness. Weight gain is prevalent, and many women with PCOS find it challenging to manage their weight due to insulin resistance.
Western Medicine Approach
In the realm of Western medicine, conventional treatments often involve hormonal contraceptives to regulate menstrual cycles and manage symptoms. Depending on the severity of the symptom, anti-androgen medications may be prescribed to alleviate hirsutism and acne. Lifestyle interventions, including dietary changes and exercise, are also emphasised to address insulin resistance within the approach of Western medicine.
Traditional Chinese Medicine (TCM) Approach
Traditional Chinese Medicine offers a holistic perspective on PCOS, addressing the underlying imbalances in the body’s energy or Qi. Acupuncture, a key component of TCM, is often used to restore the flow of Qi and promote overall well-being. Acupuncture points related to reproductive organs, hormonal regulation, and improving water metabolism via the triple energiser meridian and digestive system are targeted to free stagnant qi and alleviate and soothe PCOS symptoms.
Acupuncture looks at patterns and in the case of PCOS, the patterns are associated with damp accumulation due to Kidney yang deficiency (Dea, 2015) and/or Spleen qi deficiency.
Recent studies have implied positive respond via auricular acupuncture and vagus nerve stimulation (Zhang et al., 2023).
Herbal remedies, another integral part of TCM, are prescribed subject to the needs of the individual (Xu et al., 2023). Common herbs used by TCM to treat symptoms of PCOS include:
- Dong Quai (Angelica sinensis): Known for its hormone-balancing properties, Dong Quai is used to regulate menstrual cycles and ease cramping.
- Peony (Paeonia lactiflora): This herb has anti-inflammatory properties and is believed to regulate hormonal imbalances in women with PCOS.
- Licorice Root (Glycyrrhiza glabra): Helps in reducing testosterone levels and improving hormonal balance.
- Chinese Skullcap (Scutellaria baicalensis): Known for its anti-androgenic effects, may help manage hirsutism and acne.
The combination of acupuncture and herbal remedies in TCM aims to address the root causes of PCOS, providing a personalised and holistic approach to symptom management.
Awareness and Lifestyle Modification
Women with PCOS have sought relief through various methods, including lifestyle modifications and herbal remedies. Diets containing whole foods, fruits, and high protein play a crucial role in managing symptoms, with a focus on maintaining a healthy weight and improving insulin sensitivity. Exercises that follow a woman’s menstrual cycle also help in balancing hormones, for example, doing slower and calmer exercises such as yoga and Tai Chi during menstrual phase and follicular phase (day six to fourteen, as oestrogen and progesterone is on the rise). Conversely, during the ovulation phase, women are advised to partake in high-intensity exercise such as running and swimming as their energy levels are on the rise. Monitoring one’s hormones and partaking in activities according to the phase can help in maintaining a balance hormone levels. Herbal supplements, such as chasteberry and spearmint tea, have been used to address hormonal imbalances, too.
Conclusion
Polycystic Ovary Syndrome is a challenging condition that demands a multifaceted approach to management. There is no one set route to improve and manage this condition. Whether one choose to embrace traditional methods, or Western medicine, the key lies in seeking timely and personalised treatment, thus emphasising the need towards monitoring symptoms and getting treatment as soon as they affect the overall life of a woman. While other treatments are ideal, Traditional Chinese Medicine (TCM) uses approaches that target the symptoms and its root cause. For example, treatments will try to target excessive weight gain, mood swings, irregular menstrual cycles, excessive hair growth or even infertility. Women diagnosed with PCOS should understand that it is a manageable condition, and with the right interventions, they can lead healthy and fulfilling lives.
Regular medical check-ups, a balanced lifestyle, and a proactive attitude toward seeking help are essential for effectively navigating the complexities of PCOS. By raising awareness and promoting early intervention, we empower women to take charge of their health and well-being. Remember, PCOS is not a roadblock but a challenge that can be overcome with the right support and guidance. If you or a loved one is dealing with these symptoms, do reach out to us. At Amber and Flow Acupuncture clinic, we can assess your case and assist you to manage PCOS.
References
- Deswal, R., Narwal, V., Dang, A. S., & Pundir, C. (2020). The Prevalence of Polycystic Ovary Syndrome: A Brief Systematic review. Journal of Human Reproductive Sciences, 13(4), 261. https://doi.org/10.4103/jhrs.jhrs_95_18
- Healthdirect Australia. (n.d.). Polycystic ovarian syndrome (PCOS). Healthdirect. https://www.healthdirect.gov.au/polycystic-ovarian-syndrome-pcos
- Professional, C. C. M. (n.d.). Polycystic ovary Syndrome (PCOS). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/8316-polycystic-ovary-syndrome-pcos
- Zhang S, He H, Wang Y, Wang X, Liu X. Transcutaneous auricular vagus nerve stimulation as a potential novel treatment for polycystic ovary syndrome. Sci Rep. 2023 May 12;13(1):7721. doi: 10.1038/s41598-023-34746-z. PMID: 37173458; PMCID: PMC10182028.
- Dea, C. (2015, August 21). Polycystic ovarian syndrome and Chinese medicine — Back Bay acupuncture. Back Bay Acupuncture. https://www.backbayacupuncture.com/news/2015/5/27/polycystic-ovarian-syndrome-and-chinese-medicine
- Xu, D., Lu, M., Liu, Y., Chen, W., Yang, X., Xu, M., Zhou, H., Wei, X., Zhu, Y., & Song, Q. (2023). An Analysis of the Clinical Medication Rules of Traditional Chinese Medicine for Polycystic Ovary Syndrome Based on Data Mining. Evidence-based complementary and alternative medicine : eCAM, 2023, 6198001. https://doi.org/10.1155/2023/6198001
- Liu, J., Wu, Q., Hao, Y., Jiao, M., Wang, X., Jiang, S., & Han, L. (2021). Measuring the global disease burden of polycystic ovary syndrome in 194 countries: Global Burden of Disease Study 2017. Human Reproduction, 36(4), 1108–1119. https://doi.org/10.1093/humrep/deaa371